District Stroke Centre
Mackenzie Health is proud to be home to the York Region District Stroke Centre and a nationally accredited stroke program.
 We care for those who are either at risk of having a stroke or who have just experienced a stroke or Transient Ischemic Attack (TIA).
We care for those who are either at risk of having a stroke or who have just experienced a stroke or Transient Ischemic Attack (TIA).
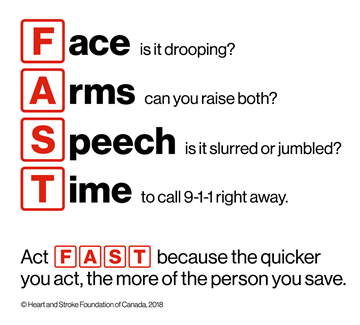
The faster you can recognize the signs and call 911, the better your chances for recovery. Calling 911 will get you to the closest hospital best suited to assess your symptoms and provide any treatment you may need.
More information can be found at the Heart and Stroke Foundation.
Patients in York Region who are having signs of stroke and fit the criteria for possible treatment are brought to Mackenzie Health by Emergency Medical Services (EMS).
As a District Stroke Centre, we are the only hospital in York Region to provide the clot busting drug called Tenecteplase (tNK) and assess eligibility to have a clot removal surgery called Endovascular Thrombectomy (EVT). Patients who are eligible to receive tNK are given this drug at Mackenzie Health. Those who are eligible for EVT are sent to an EVT-capable site like Sunnybrook Health Sciences Centre for further assessment.
Once all emergency treatments are completed, patients are moved to a hospital that offers specialized stroke care closest to their home.
The District Stroke Centre strives to provide best practice acute care, stroke rehabilitation and stroke prevention services to patients in our community and supports other hospitals in York Region to do the same. We are fully accredited by Accreditation Canada and have earned the highest designation possible, Accreditation with Distinction. Accreditation Canada is an independent non-profit organization that conducts evaluations based on well-established standards of excellence in health care. This rigorous assessment validates Mackenzie Health’s commitment to delivering reliable, safe and excellent patient care.
For more information about our program, please call the District Stroke Coordinator at 905-883-1212 extension 6215 or the Patient Care Coordinator at 905-883-1212 extension 3899.
- We proved best practice stroke care at all transitions in care along your stroke recovery journey.
- We provide patient and family centered care
- We have a robust interprofessional team that assists our patients to reach their optimum level of function and facilitate re-entry into the community safely
- We provide leadership and support to our community hospital partners in advancing stroke care throughout York Region and beyond
- We adhere to the Canadian Stroke Best Practice Guidelines
- We strive to ensure the right patient is in the right bed at the right time
- We place an emphasis on stroke prevention across the continuum of care.
TIA / Stroke / Neurology Clinic
- We provide rapid access to assessment and investigation of the underlying cause of Transient Ischemic Attack/Minor Non-Disabling Stroke (TIA/MNDS).
- We initiate interventions based on current best practices to address risk factors and the underlying cause, working in a timely manner to prevent a future stroke.
- We provide education on lifestyle and risk management, stroke prevention and warning signs for stroke.
- We facilitate referral of appropriate patients to local cardiovascular rehabilitation services for ongoing secondary prevention and chronic disease management.
- We facilitate linkage to community programs for secondary prevention and chronic disease management.
Hyper-acute
- We provide timely access to diagnostic testing
- • We provide thrombolysis (tNK) to eligible patients within 30 of arrival to the Emergency Department
- We screen patients to determine eligibility for Endovascular Thrombectomy (EVT)
- We transfer eligible patients to EVT delivery centres as quickly as possible
- We refer all patients with TIA/MNDS not requiring admission, to a Stroke Prevention Clinic like our. TIA/Stroke/Neurology Clinic.
Acute
- We provide all patients with stroke access to evidence-based stroke care
- We provide initial inter-professional assessment of all patients admitted with stroke within 48 hours
- We strive to minimize complications of stroke through the use of validated screening tools: Acute Stroke Dysphagia Screen (ASDS); Morse Falls Scale; Braden Scale Skin Assessment; PHQ-9 Depression screening; continence assessment; and cognitive assessment
- We initiate secondary stroke prevention through education and support with lifestyle changes, risk management and administration of recommended secondary prevention medications
- We follow evidence-based clinical pathways
- We ensure all stroke patients have access to rehabilitation based on standardized criteria and assessment tools including the AlphaFIM®.
Rehabilitation
- We provide all patients with stroke access to evidence-based stroke care
- We provide timely initial interprofessional assessment of all patients admitted with stroke aligned with most recent best practice recommendations
- We complete the Functional Independence Measure (FIM)® on all patients within the first three days of admission to rehabilitation in order to determine a baseline level of function. This assessment is re-administered upon discharge to assess changes in function
- We provide best practice interprofessional rehabilitation, tailored to each patients' needs and functional goals
- We use evidence-based techniques and equipment to ensure optimal therapeutic value and achieve optimal outcomes
- We hold weekly education for patients and families to help them prepare for their transition out of hospital
- Our interprofessional team includes a physiatrist - a doctor who is a specialist in physical medicine and rehabilitation
- We provide instruction to families and caregivers in an effort to promote carry-over of rehabilitation concepts and techniques
- We initiate secondary stroke prevention through education and support with lifestyle changes, risk management and administration of recommended secondary medications.
Community Reintegration
- We provide seamless transition back into the community through a comprehensive discharge planning
- We refer all eligible patients to a Stroke Prevention Clinic (see TIA / Stroke / Neurology Clinic) for follow-up and, if indicated, will initiate a referral to Cardiovascular and Pulmonary Rehabilitation
- We provide accessible information to all patients and their family members regarding community resources
- We initiate referrals for all patients requiring outpatient rehabilitation and/or other community services
- We support and inform planning of community services that address current gaps in stroke care across York Region and Central LHIN.
Sorbara Integrated Stroke Unit - Inpatient Stroke Services
For Information about Stroke Inpatient Services Contact Patient Care Manager or Patient Coordinator
905-883-1212 ext. 3899
fax 905-883-0772.
Mackenzie Richmond Hill Hospital
TIA/ Stroke/ Neurology (TSN) Clinic
A-Wing, Level 1, room 100
10 Trench Street
Richmond Hill, ON L4C 4Z3
Local to Richmond Hill: 905- 883-1212 ext. 7721
Local to Vaughan: 905-832-4554 ext. 7721
Fax: 905-883-2246
View the map for this location
District Stroke Center
For Information about stroke services in York Region and Education Outreach in the community Contact the District Stroke Centre: 905-883-1212 ext. 6215
Groups wishing to host a stroke awareness event please contact anna.sewell@mackenziehealth.ca